Air pollution, stress contribute to low-birth-weight babies for L.A. Latinas, study finds
Infants with low birth weight face increased risks of mortality and a multitude of long-term health troubles.
Fetal growth — which is delicate and precisely programmed — may be disrupted by a mother’s exposure to air pollution and psychological stress during early to mid-pregnancy, a new USC study shows.
The findings, published Tuesday in JAMA Network Open, suggest that protecting pregnant women from air pollution may improve birth weight, especially among stressed-out mothers living in environmentally burdened neighborhoods.
“Although air pollution has a harmful effect on many different populations, our study identified the effects on expectant mothers who are already most vulnerable,” said Zhongzheng “Jason” Niu, postdoctoral scholar and research associate at the Keck School of Medicine of USC and the study’s first author.
“The addition of high perceived stress is another factor contributing to this issue. We already know air pollution is linked to low birth weight and future disease risk. Protecting pregnant women from these risks would ultimately protect future generations.”
Newborns with low birth weight face increased risk of neonatal mortality and potential complications such as breathing problems, bleeding in the brain, jaundice and infections. Low birth weight is also associated with long-term disease risks including diabetes, heart disease, high blood pressure, intellectual and developmental disabilities, metabolic syndrome and obesity.
Stress, air pollution and newborns: identifying at-risk mothers
Data from 628 predominantly low-income Hispanic women pregnant with a single baby was collected between 2015 to 2021 as part of USC’s MADRES (Maternal and Developmental Risks from Environmental and Social Stressors) Center.
(Story continues below graphic)
Patients were recruited primarily from Eisner Health in downtown Los Angeles and the Los Angeles County+USC Medical Center prenatal clinic. Biospecimen data, medical records and residential information were collected during clinic visits. Participants completed a Perceived Stress Scale questionnaire to gauge their perceptions of stress. Their neighborhood-level stressor was measured by the CalEnviroScreen Score, a California statewide screening tool to identify neighborhoods that have been disproportionately burdened by multiple sources of pollution and population vulnerability.
The average age of participants was 28 years; 73% self-identified as Hispanic and 32% listed Spanish as their preferred language. Twenty-one percent of the mothers reported high levels of stress in their lives. More than 60% of the participants lived in a neighborhood with a CalEnviroScreen Score greater than 50, indicating a high cumulative burden.
Microscopic particles threaten developing babies
Three components of polluted air were examined: PM2.5, PM10 and NO2. Levels of the pollutants were monitored from ambient air quality data (U.S. Environmental Protection Agency Air Quality System) with an average of four monitoring stations within about 5 to 9 miles of each participant’s residential address.
Emissions from the combustion of gasoline, oil, diesel fuel or wood produce particles of PM2.5, which have a diameter of 2.5 micrometers or less — 30 times smaller than a strand of hair. PM10 has a diameter of less than 10 micrometers and can be found in dust and smoke.
NO2, nitrogen dioxide, is another pollutant released when fossil fuels are burned at high temperatures.
Daily estimates of 24-hour average NO2 and particulate matter were assigned to each participant’s residential location, from 12 weeks before conception to 36 weeks into pregnancy.
Conclusions from study on stress, air pollution and babies
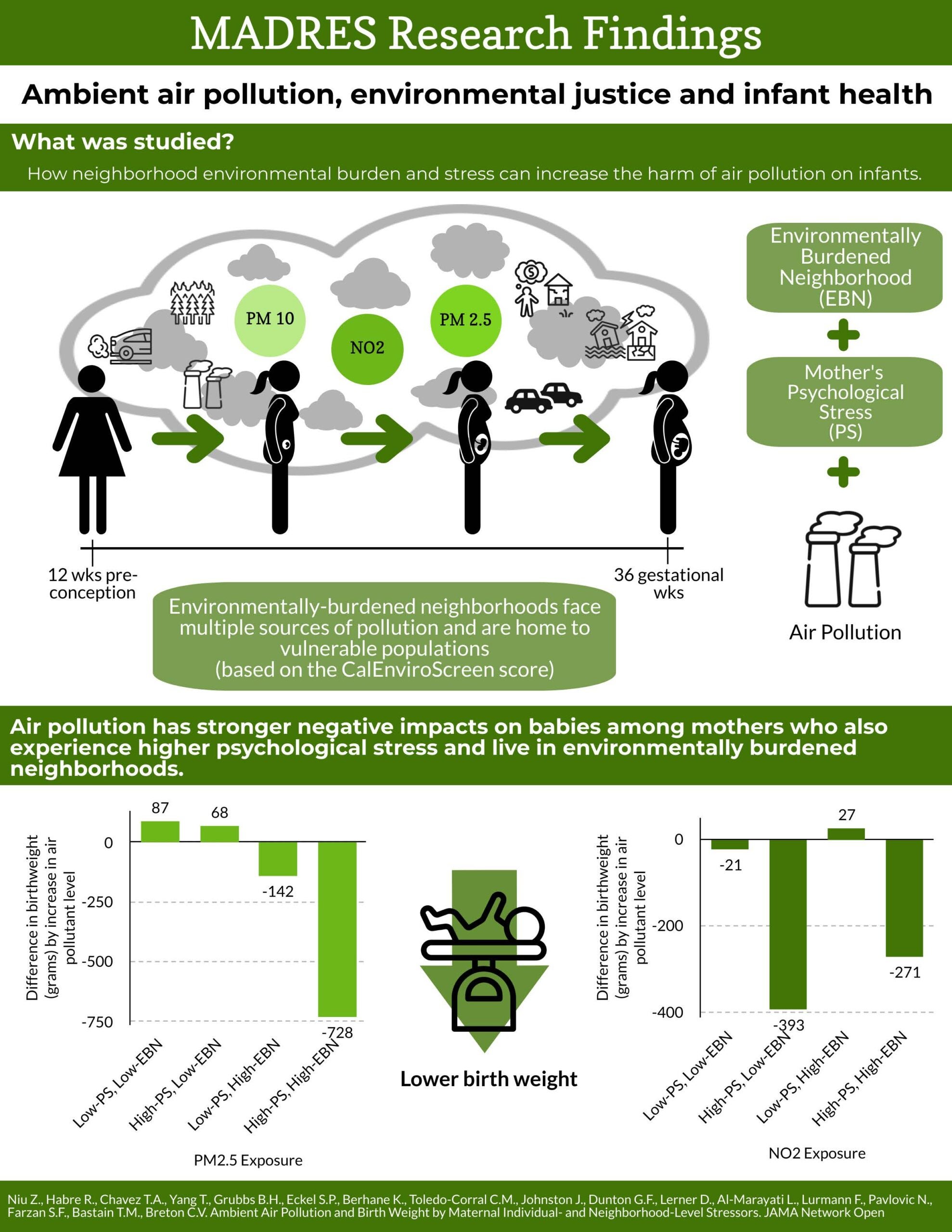
Exposures to particulate matter and nitrogen dioxide in early to mid-pregnancy are significantly associated with lower birth weight, researchers found. On average, birth weight was 9.5 grams lower each interquartile range increase (4 µg/m3) of PM2.5 exposure during the 14- to 22-week gestational period.
Even more concerning, mothers with high stress scores who also live in the most environmentally burdened neighborhoods experienced greater decreases in birth weight. In this group, mothers exposed to the highest levels of PM2.5 at four to 20 weeks delivered babies weighing 34 grams, or 1 ounce, less in birth weight and mothers exposed to highest PM10 at nine to 14 gestational weeks delivered babies weighing 39.4 grams less, on average.
Despite reductions in air pollution in California, we are still seeing harmful effects of air pollutants on birth weight … in vulnerable populations.
Carrie Breton, Keck School of Medicine
In the same group, exposure to NO2 from nine to 14 gestational weeks was associated with a 40.4-gram decrease in birth weight. Exposure at 33 to 36 gestational weeks reported the greatest decrease in birth weight: 117.6 grams, or 4.1 ounces.
“Despite reductions in air pollution in California, we are still seeing harmful effects of air pollutants on birth weight, a key indicator of baby’s future health, in vulnerable populations,” said last author Carrie Breton, a professor of population and public health sciences at the Keck School of Medicine. “The most vulnerable women are those who are hit with multiple types of stressors, and experience stress in different ways. The combination of stressors and pollutants is important to consider in protecting babies’ health. Continuing to monitor air pollutants still needs to be a priority. Reducing individual and neighborhood stressors should also be a priority, particularly at the policy level.”
About the study: In addition to Niu and Breton, other authors of the study include Theresa M. Bastain, Thomas A. Chavez, Genevieve F. Dunton, Sandrah P. Eckel, Shohreh F. Farzan, Rima Habre, Jill Johnston, Claudia M. Toledo-Corral, Tingyu Yang of the Department of Population and Public Health Sciences, Keck School of Medicine, University of Southern California; Laila Al-Marayati and Brendan H. Grubbs, Department of Obstetrics and Gynecology, University of Southern California; Kiros Berhane, Department of Biostatistics, Mailman School of Public Health, Columbia University; Deborah Lerner, Eisner Health Los Angeles; and Fred Lurmann and Nathan Pavlovic, Sonoma Technology Inc.
The research was supported by NIH grants P50MD015705, P50 ES026086, UH3OD023287, P30ES007048, R01ES027409 and EPA grant 83615801–0.



